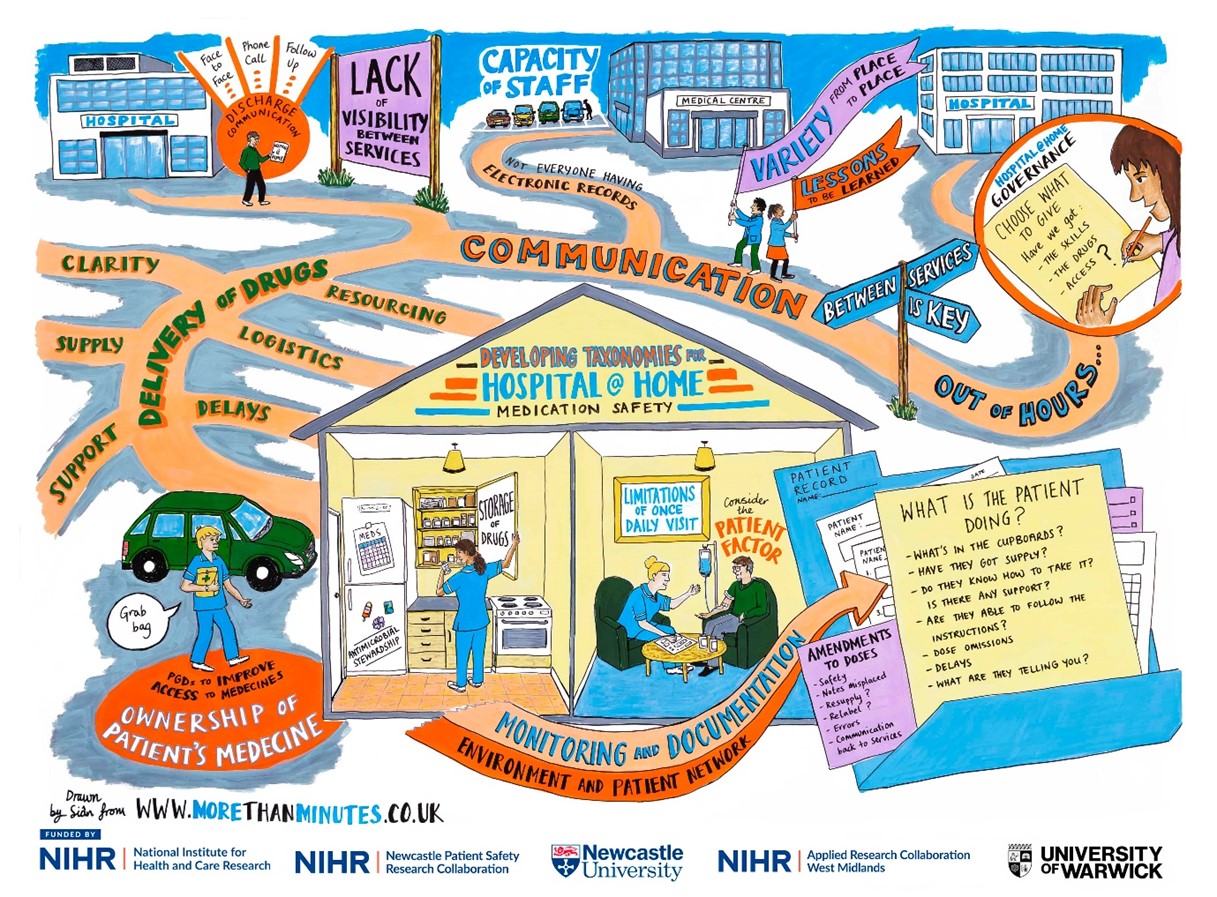
Figure 1 above
How it all began?
I remember attending my first Hospital at Home Society conference in 2024. At this point, I was in the early days of the PhD, eager to learn more about current developments in this research area. During the networking breaks, I remember introducing myself to keynote speakers and little did I know that this would be the start of a wonderful collaboration and supervision for the NIHR SPARC Award.
I was keen to discuss the priority research areas for Hospital at Home (H@H) and later that year, I came across the NIHR SPARC Short Placement Award for Research Collaboration | NIHR. I felt that this was a wonderful opportunity to work with a research team that had the expertise in H@H, who operationally had the research knowledge, the technical and practical expertise in this field, and the existing networks that I could learn from and engage with moving forward. Additionally, my aspirations for professional development to become a clinical academic drove my passion to work with a group of dedicated and trailblazing clinical academics. I felt this would strengthen my experience, especially when considering post-doctoral opportunities.
What is the SPARC award for?
The NIHR SPARC Award allows NIHR academy members to spend time with researchers across other NIHR infrastructure to enhance their personal and professional development and research training experience. From speaking to previous candidates, I learned that this is usually either to develop skills in particular research methods, or to develop collaborations and expertise from researchers in a particular field.
What I did?
The application itself allows you to be quite flexible in how you undertake the placement, which is helpful depending on what you want to achieve. Personally, I had set out 1 day a week over 9 months, whereas other previous applicants undertook it in block placements (e.g. in a 4-week block).
During the placement I managed to conduct clinical visits to H@H services to get the first-hand practical experience. I attended clinical meetings and research meetings linking in with other health tech research centres in the NIHR infrastructure. As part of the award, I also accounted for attending courses and conferences around implementation science and knowledge mobilisation which I felt would be useful for my professional development and demonstrating meaningful impacts with research. The bulk of the collaborative work centred around working on a multi-phase research project. This involved a literature review and arranging an online stakeholder workshop with clinical experts nationally to discuss the findings. This also involved working with a visual minutes artist and presenting the findings at the UK Hospital at Home Society Conference 2026, at the Royal College of Physicians in Edinburgh, which supported input into the survey with H@H practitioners.
Outputs of the placement?
This placement allowed us to develop a Taxonomy of Medicines Safety in Hospital at Home which is aimed for upcoming publication. This enables a better understanding of the concepts of medicines safety in H@H and the links between them. Although the aim of the placement is professional development, I was fortunate to have an abstract accepted for oral presentation at the UK Hospital at Home Society conference in 2026, which is planned for submission to the Journal of Advanced Home Medicine. Additionally, a visual minutes graphic produced from this work is displayed below (See Figure 1).

Blog produced by Faiza Yahya (PhD Candidate), with acknowledgements to the support and supervisory team at the University of Warwick (Professor Daniel Lasserson, Dr Ciara Harris, Sophie McGlen) and the NIHR for funding this award. Appreciation also goes to the Academic Career Development Leads (Newcastle University and NIHR ARC West Midlands) for making this happen.
When “help” might harm: understanding the safety of social prescribing
Social prescribing has become a cornerstone of person-centred care, connecting people to community support, reducing pressure on services, and improving wellbeing. But what happens when these interventions don’t go as planned?
In our recent study, we looked beyond effectiveness to explore an underexamined issue: the potential harms of social prescribing. Using a global umbrella review of existing evidence, we developed a “dark logic” model (a way of mapping how unintended negative consequences might arise).
What did we find?
While social prescribing can offer important benefits, the evidence base highlights several areas of potential risk:
- Mismatch between needs and services – when referrals don’t align with individual circumstances, leading to frustration or disengagement
- Equity concerns – where access to community resources is uneven, potentially widening inequalities
- Burden transfer – shifting responsibility onto individuals or overstretched voluntary sector services
- Psychological impacts – including feelings of stigma, rejection, or failure if support pathways break down
Importantly, many of these harms are not the result of single decisions, but emerge through complex systems of care, commissioning, and delivery.
Why this matters for patient safety
Patient safety conversations have traditionally focused on clinical interventions. Our findings suggest we need to extend that thinking into community-based and non-medical models of care.
Social prescribing operates across organisational boundaries (primary care, local authorities, and the voluntary sector) which can create gaps in oversight, accountability, and follow-up. Without careful design, implementation, and evaluation, there is a risk that well-intentioned interventions could inadvertently contribute to harm.
What can we do differently?
Our “dark logic” model is not about discouraging social prescribing, but about making it safer and more equitable. Key implications include:
- Building safety considerations into service design from the outset
- Strengthening monitoring of outcomes beyond uptake and satisfaction
- Supporting the voluntary and community sector to deliver sustainable services
- Ensuring equity is a central focus in referral pathways and access
- Recognising and addressing the emotional and psychological experiences of participants
Looking ahead
As social prescribing continues to grow, there is an important opportunity to embed patient safety principles into its development. This means moving beyond asking “does it work?” to also asking “for whom, in what contexts, and at what cost?”
By bringing a safety lens to this evolving area of practice, we can better ensure that social prescribing delivers on its promise, without leaving unintended harms unseen.
Call to action
We encourage researchers, practitioners, commissioners, and community partners to actively incorporate safety thinking into social prescribing policy and practice. This includes:
- Designing services with potential harms in mind, not just intended benefits
- Sharing learning on unintended consequences across organisations and sectors
- Embedding routine monitoring of safety outcomes in evaluation frameworks
- Involving patients and communities in identifying what “safe” support looks like in practice
By working collaboratively and proactively, we can ensure that social prescribing not only supports wellbeing, but does so safely, equitably, and sustainably.
Paper link – https://bmjopen.bmj.com/content/16/5/e108998.abstract
Dr Matthew Cooper
Perspectives from the PSRC Newcastle, Disadvantaged Communities Theme were included in a new report from Bowel Cancer UK on cancer diagnoses in hospital emergency departments – which is the foundation of a new campaign by the charity on this topic.
This patient insight report is an important first step in understanding the experiences of people and families affected by emergency bowel cancer diagnoses. Hearing these perspectives helps us appreciate the emotional and practical impact on patients and their loved ones, while also beginning to identify areas where improvements could make a real difference.
Connecting experiences from both patients and professional viewpoints helps us develop a complete picture of what happens, what is working and what may need to change. This comprehensive understanding is the first step in making sure that future interventions are grounded in real experiences and, ultimately, that patients and families are better supported.
Please follow the link below to read the full report:

Pippa Wood NIHR Newcastle PSRC Operations Manager
I went to the NIHR SafetyNet Organisational Culture working group meeting in Birmingham on a cold day in January. I wanted to learn what “organisational culture” means and how it links to patient safety.
So, what is organisational culture?
After listening to researchers from different PSRCs, I learned that organisational culture is basically how people at work get along. It includes the relationships between colleagues, managers, departments, services and different job roles.
How does this affect patient safety?
The way people treat each other at work can directly affect the care patients receive. If communication and relationships between teams are poor, things can go wrong.
For example:
- A patient might be sent home from hospital, but no one tells their family or carers, so no one is there to meet them.
- A family may still be waiting for a call to say they can collect their loved one, only to find out the patient has already been taken home by hospital transport.
But when communication and teamwork are good, patients get much better care.
For example:
- Maternity staff might tell new mothers about breastfeeding support available in their community.
- If an older person is having surgery, hospital staff may work with community care teams and family members to plan what help the patient will need at home.
The biggest thing I learned
If staff are unhappy, feel unappreciated, experience bullied, or feel insecure in their jobs, this can lead to poor communication and bad relationships at work. This can then cause poor-quality services, lower standards of care, and higher risks to patient safety.
But if staff feel happy, valued, and supported, they are more likely to work well together. Good relationships between teams mean better services, higher standards of care, and safer experiences for patients.

Dr Matthew Cooper, NIHR Newcastle PSRC Safer Integrated Health and Social Care Environments, Research Associate
Dr Matthew Cooper, NIHR Newcastle PSRC Safer Integrated Health and Social Care Environments, Research Associate
Broadening My Understanding of Organisational Culture
Attending the organisational culture working group helped me to broaden my understanding of what organisational culture truly represents. Initially, I viewed workplace culture mainly in terms of supporting staff wellbeing and keeping people happy and healthy at work. Through the discussions, I realised how strongly organisational culture also influences patient safety and the consistent delivery of high-quality care.
Exploring the Ambition of the 10‑Year Plan
The working group explored the ambition of the 10-year plan, which is expected to drive change both during the next 10 years and for the future beyond. This however highlights some key risks:
- That pressure to deliver quickly could lead to rushed decisions,
- Missed input from some disciplines (implementation science for example), or
- Action being taken without full consideration of the plausible impacts (for example removing resources from one service to fund a new idea).
A strong emphasis was placed on transparency of quality of care, including empowering patients through greater voice, choice and access to information. This was balanced alongside clearer accountability and stronger incentives for high-quality care. I was particularly struck by the challenge of double running costs, where services must continue to operate while resources are reallocated, and the importance of deliberately creating time for safety within this context.
Reaffirming the Core Purpose of Organisational Culture
Overall, the working group reinforced that the core goal of organisational culture is to support patients, underpinned by robust checks and balances, compassionate leadership, and a shared commitment to quality and safety at every level of the system. As a team at the NIHR Newcastle PSRC, this is something we are all hoping to reflect on and take forward in our research.
Learn more about the NIHR 10 year plan.
by Nathania Bestwick NIHR Newcastle PSRC PhD student
I was grateful to travel to London for the PSYCH Symposium 2025 on Thursday, 4th December. This symposium brings together researchers, therapists, doctors, policymakers, investors, and campaigners to talk about the latest research in psychedelic medicine and how psychedelic therapies may be used in mainstream healthcare to treat mental health conditions.
I attended the symposium with Radin Karimi, another PhD student from the NIHR Newcastle Patient Safety Research Collaboration (PSRC). Like my own work, Radin’s research looks at how to better manage polypharmacy (which is when people take many different medicines at the same time). Medicines used to treat mental health conditions often add to this problem, so we were interested to find out if psychedelic therapies might help people manage their mental health so they can take fewer medicines. We were also keen to learn how patient safety is managed in this developing area of research.

The symposium focused on a range of conditions, including depression, anxiety, PTSD, addiction, eating disorders and distress near the end of life, particularly for people who have not responded to more commonly used treatments. Speakers shared evidence showing that psychedelic medicine, such as psilocybin, MDMA and ibogaine, can help to ease symptoms in people with these conditions. They also explained that psychedelic therapies may help people process deeper emotional problems behind their symptoms, which can lead to longer-lasting improvements in well-being. Several speakers had worked with military veterans and shared how these therapies have helped them manage PTSD, support their mental health, and feel better in everyday life after leaving the military.
Patient safety was a major focus throughout the symposium. Research in this area is strictly regulated, with people being carefully checked (called screening) before they’re invited to take part, and with study information being clearly explained so that people can make an informed choice when agreeing to join a study. Therapies are provided in carefully controlled and supportive treatment spaces by highly trained therapists and healthcare professionals, with close monitoring during sessions, and follow-up support after the treatment to help people understand their experiences and get the best results from the treatment.

Professors David Nutt and Guy Goodwin had an interesting discussion about recent results from a large study which showed that a single dose of synthetic psilocybin helped people with severe, long-lasting depression, with higher doses leading to bigger improvements in symptoms. They also spoke about drug laws creating stigma around psychedelic research, even though there is growing evidence that these substances can have real health benefits and that they may be less harmful than legal drugs, such as alcohol and tobacco.
One example of how psychedelic medicine is being used in standard healthcare came from Professor Ranil Gunewardene, who described how he is leading one of the first clinics in Australia to offer regulated psychedelic-assisted therapy. Since his research is with patients who have complex health conditions (called real-world patients), it may give us helpful insight into how these therapies can be used outside of highly controlled research environments.
In summary, the symposium showed that psychedelic medicine has promising potential to improve care for people with mental health conditions, particularly those that are difficult to treat. It also highlighted that more research is needed and that building upon the current evidence base will help us better understand how effective and safe these treatments are, and how they can be carefully and appropriately used as part of standard healthcare.
Details and bios for each of the speakers can be found here
Yahya F, Cooper M, Saif W, Kassem M, Nazar H Development of a Hospital at Home Digital Twin for Patients With Frailty: Scoping Review Journal of Medical Internet Research 2025;0:e0 URL: https://www.jmir.org/2025/1/e81510 doi: 10.2196/81510
What’s this about?
How can we make the most of advanced technology and live information to improve how we deliver hospital-level care at home?

What’s this about?
How can we make the most of advanced technology and live information to improve how we deliver hospital-level care at home?
Why are we looking at this?
The NHS 10-year plan wants to:
- Move more care from hospitals closer to home
- Prevent illness instead of just treating it
- Use more digital tools to support care

What is the work we are doing?
We explore all three by using something called Digital Twins. A Digital Twin is like a live virtual simulation of a patient and their surroundings using real-time information. It can help healthcare professionals predict problems early, to give care that’s safer and more personalised.
Learning from, and working with other experts, our work looked at creating a simple step-by-step model, which can be used to develop a Hospital-at-Home Digital Twin. This review was based on existing evidence for tools to support this, for patients living at home with frailty.
What does this mean?
- Technology and real-time data can help health professionals care for patients at home more efficiently.
- Digital Twins could make care timelier, safer, and tailored to each person.
- We’ve outlined the main building blocks for creating a Hospital at Home Digital Twin.
This work is just the beginning, but it shows how technology could possibly change the world of healthcare and what needs to be worked on to make this possible.
For those that want to know more:
Our article reviews the current evidence for tools that exist to support the development of a Hospital at Home Digital Twin. We describe the 5 layers required to build a Digital Twin. Results show that a variety of technologies exist to pick up information, such as wearables. However more understanding is needed of how we manage that data, store it, translate it and use it to make useful predictions to help staff who are looking after us make decisions. This article also talks about some of the challenges and opportunities we may face when using these technologies in our current healthcare system.

By PhD Student Jess McCann
For our October EDI event we welcomed Steve Storey, lead clinical pharmacist at Cumbria, Northumberland, Tyne & Wear (CNTW) NHS Trust, to come and speak to us about how we can make ‘Reasonable Adjustments to create Inclusive Consultations for Patients’.
Reasonable adjustments are described as small, sensible changes made so that people who face barriers to accessing and receiving care, due to a disability, mental health condition or other additional needs, are given equal opportunities.
He explained that we accept reasonable adjustments (like physical ramps, interpreters and assistive technology) in many areas of day-to-day life, so why should healthcare consultations be any different? Within healthcare settings, failing to make such adjustments could worsen existing inequities. For instance, people with un‐met communication, sensory or cognitive needs may experience worse outcomes, including higher mortality, simply because the system assumed a “one size fits all” approach.
In Steve’s session, he spoke of examples of what counts as “reasonable” vs. “unreasonable” adjustments. Sometimes, it isn’t about removing all risk or achieving perfect equality in consultation duration and structure, but about taking practicable, proportionate and effective steps to address disadvantages for that person, at that time. He then moved into an interactive exercise with the audience to experience some of the disadvantages people may face. He asked us to solve a complex mental‐math calculation within 30 seconds; then to try reading some text in a different language; then to try reading very small, blurry text. These simple activities illustrated how patients with cognitive impairment, language barriers, sensory loss or low health literacy are at a disadvantage when seeking, accessing or receiving health care. It was eye-opening to experience the frustration, the delay and confusion that patients are subject to.
Steve discussed several barriers for patients accessing care, such as language and language style, communication that isn’t just about language (e.g., neurodiversity, sensory needs, memory, processing speed), physical disability, diagnostic overshadowing and hypersensitivity (e.g., to sensory stimuli, environments, noise, smells). These may mean that reasonable adjustments to consultations are used; for example, longer appointment times, quieter environments, visual prompts, alternative formats, consultation breaks or bringing a support person to accompany.
Steve shared with us some very impactful real-life examples of people he has provided care for who have required reasonable adjustments, and demonstrated what it means to go the extra mile in delivering person-centred care.

He summarised that reasonable adjustments are not something necessarily taught within university or professional training but are central within professional capability. Being aware of additional needs, asking patients what they would prefer and anticipating barriers and how to act on them allows us to demonstrate humility and advocate for the best possible outcomes for our patients.
It was a very stimulating and thought-provoking session, and it was great to see a big audience of attendees, spanning undergraduate Pharmacy students, postgraduate students, members of the NIHR Newcastle PSRC, wider University network and clinical colleagues from Newcastle upon Tyne Hospital NHS Foundation Trust. The talk provided valuable insights that we can apply not only in our current roles but also take with us throughout our future careers. Engaging with reasonable adjustments in consultation settings may allow us to be better equipped to promote person-centred care to diverse, underrepresented patient groups.
Thank you, Steve!


By Hiranmayi Madabhushi Hari, Research Assistant (School of Pharmacy)
Equity cannot exist without disability inclusion. This month, as we mark UK Disability History Month, I want to pause and reflect on what inclusion really means, beyond statements, beyond awareness posts and beyond checkboxes on institutional forms.
Disability is not a niche issue. It is a public health issue.
It is a human rights issue.
It is a societal responsibility.
Disability history reminds us that progress did not happen by accident. It came from disabled activists demanding better-from accessible transport to inclusive education, to rights-based healthcare. Their work continues today, and we owe it to them to keep pushing.
Across the world, disabled people continue to face overlapping barriers such as inaccessible healthcare, limited education and employment opportunities and stigma that is often disabling than the condition itself. Out of the barriers they face, the most difficult one which sits uncomfortably at the intersection of public health, ethics and disability rights is the emergence of measures that subtly suggest a final option when what is most urgently needed is meaningful prioritisation, adequate resourcing, and sustained approaches that uphold the value of their lives.
True accessibility is not an afterthought. It is a starting point. It asks us to design spaces, policies and services that recognise disability as a natural part of human diversity, not an exception or burden to accommodate. The answer to our questions must always be better care.
This month, I hope we move from awareness to action.
From support to taking accountability.
From Inclusion to redesign.
Because a society that works for disabled people works better for everyone.
To all disabled students, staff, parents, carers and community members- your presence strengthens the world, your voices reshape our understanding, and your contributions enrich our collective future.
Let’s honour Disability History Month not just by remembering the past, but by reshaping the future together.
By PhD Student Liyuan Zhu
On 17th October 2025, I was very excited to present my research poster at the NIHR SafetyNet Symposium in Manchester. SafetyNet is a group of six NIHR Patient Safety Research Collaborations (PSRCs) across England. This year’s event had a special theme: “Tackling Inequities in Patient Safety.” It was the first time to bring together researchers, doctors, and patient representatives from across the country to share ideas and thoughts.
The symposium included inspiring talks, research showcases, discussions, and poster sessions. I was especially interested in two keynote talks, one about moving away from a “blame culture” in healthcare, and another about ethnic inequalities in patient safety.
I also learned about many areas I had never thought deeply about before, such as healthcare harms in prisons, inequality in perioperative and respiratory care, and access to medicines for people experiencing homelessness.

These sessions made me realise that inequality in health is a very complex issue. It is shaped by factors like race, social background, environment, and language, and also by how society responds to unfairness itself. These issues are linked together, often trapping those already at a disadvantage. To change this, what we can do is to build a strong “safety net” that supports everyone, especially people who are underrepresented or face extra barriers.

My poster was titled “Predicting Diabetic Eye Disease with AI: Trajectory Embedding and Causal Exploration of Statin Effects.” In simple terms, my study looked at how artificial intelligence (AI) can help predict who might develop diabetic eye disease, a leading cause of sight loss in people with diabetes. I also explored whether statins, common cholesterol-lowering medicines, can help reduce this risk. In addition, we found that there are inequalities between males and females, and among diabetes types. These results suggest that healthcare can be more personalised and fairer for each person.
Attending this symposium was a great experience. I met many passionate researchers who share the same goal: to make healthcare safer and more equal. It reminded me that technology like AI should not only make predictions but also help reduce health inequalities and improve care for everyone.
By Kamil, NIHR Newcastle PSRC Patient, Public Contributor
Lured by the promise of good food and new acquaintances, on Friday 17 October I made my way to Manchester for the NIHR SafetyNet Symposium – a gathering of clinicians, researchers and public contributors united by a single mission: tackling inequities in patient safety. Hosted by the Greater Manchester Patient Safety Research Collaboration (PSRC), the event brought together colleagues from the six PSRCs across England – Central London, Greater Manchester, Midlands, Newcastle, North West London and Yorkshire & Humber.
The day began with coffee and a bustling lobby filled with poster presentations. From the start, it was clear this wasn’t just an academic exercise. It was a collective effort to bridge the gap between policy, practice and lived experience.
One of the first things that struck me was the keynote by Dr Rosie Benneyworth from the Health Services Safety Investigations Body (HSSIB). I hadn’t heard of HSSIB before and I found its mission fascinating. The organisation investigates systemic issues in healthcare topics such as sepsis, prison health and fatigue without focusing on blame. Instead, it looks for learning and improvement. This shift from a ‘who’s to blame’ culture to one of collective accountability resonated deeply with me.
A presentation on avoidable healthcare-associated harm in prisons was another eye-opener. While I wasn’t surprised to hear that prisoners and people experiencing homelessness suffer significantly worse health outcomes, it was sobering to see how these inequities manifest in daily practice e.g. medication shortages, missed appointments and institutional barriers that make basic care difficult. As someone finishing reading a book on health promotion, I could connect the dots between theory and reality: these are not abstract inequalities, they are lived injustices.

One reflection that stayed with me came from a discussion about adoption and breaking cycles of poverty and violence. Even in systems that often feel broken, there are ways to create safety and opportunity through compassion and action.

Several sessions focused on the intersection of communication and safety, including translation and interpreting services. This hit particularly close to home. As a qualified Polish interpreter, I know how vital accurate translation is for patient safety, yet the pay rates offered by NHS providers are often so low that professionals can’t afford to take the work. Hearing that language access was being discussed as a safety issue, not just a convenience, was both encouraging and frustrating. We have the knowledge; now the system needs the will to act.
The Patient Safety Healthcare Inequalities Reduction Framework, presented by Dr Hester Wain, outlined five principles for change: communication and information, training and resources, data, co-production, and research. I was especially struck by her emphasis that the experiences informing the framework are what make it powerful.
By the end of the day, after many conversations in the poster corridor and a moving talk on ethnic inequities in patient safety by Professor Dawn Edge, I left Manchester feeling both hopeful and challenged. The message was clear: health doesn’t happen in a vacuum. Tackling inequity requires empathy, collaboration, and, above all, a commitment to listen to those whose voices are too often ignored. For me, as a patient-cum-public contributor, the symposium was a reminder that my lived experience isn’t just welcome in research – it’s essential.

